Blood Sugar Balance
One of the most powerful tools I use personally and clinically is a continuous glucose monitor (CGM).
Why?
Because blood sugar instability is one of the most common hidden drivers of:
• fatigue
• hormone imbalance
• cravings
• stubborn weight gain
• sleep disruption
And women often experience more fluctuations due to hormonal shifts across the menstrual cycle.
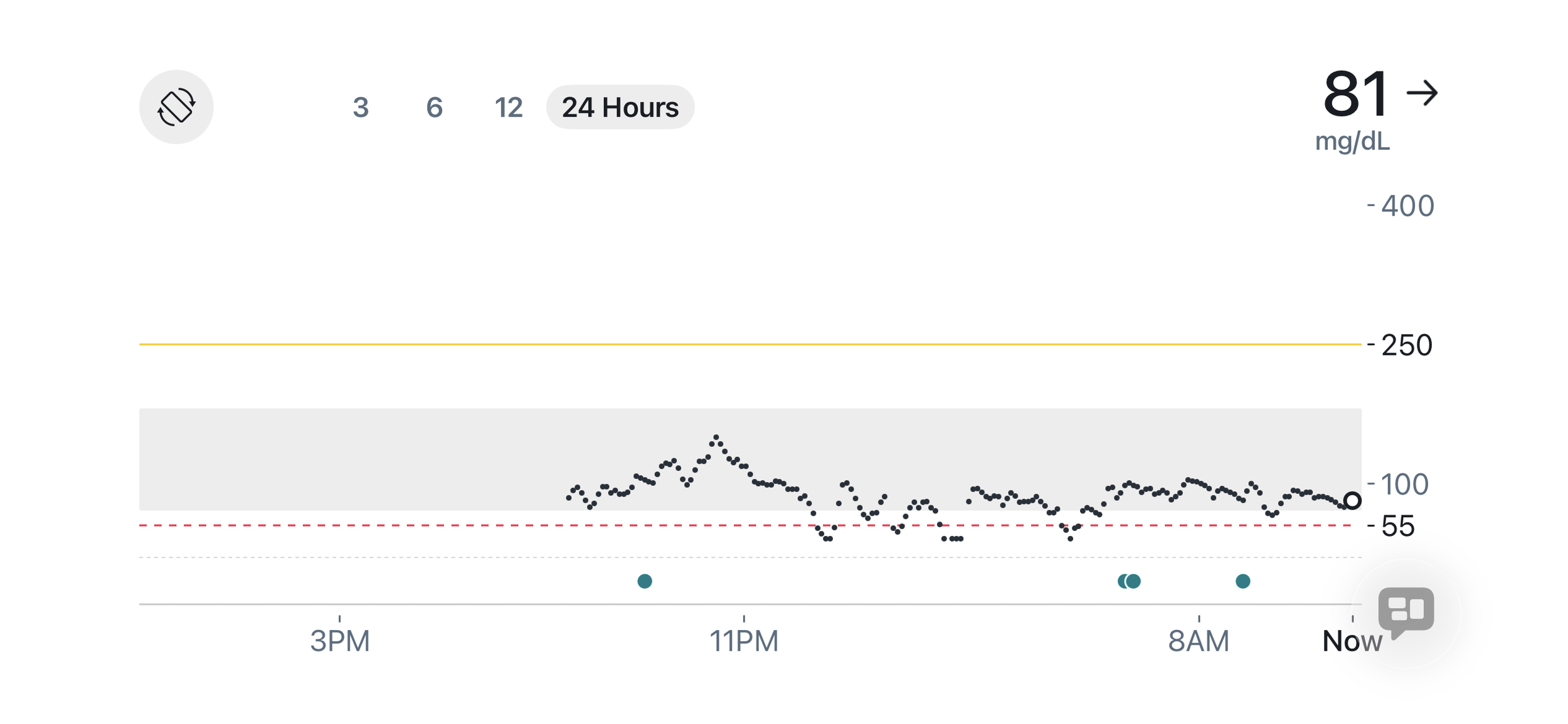
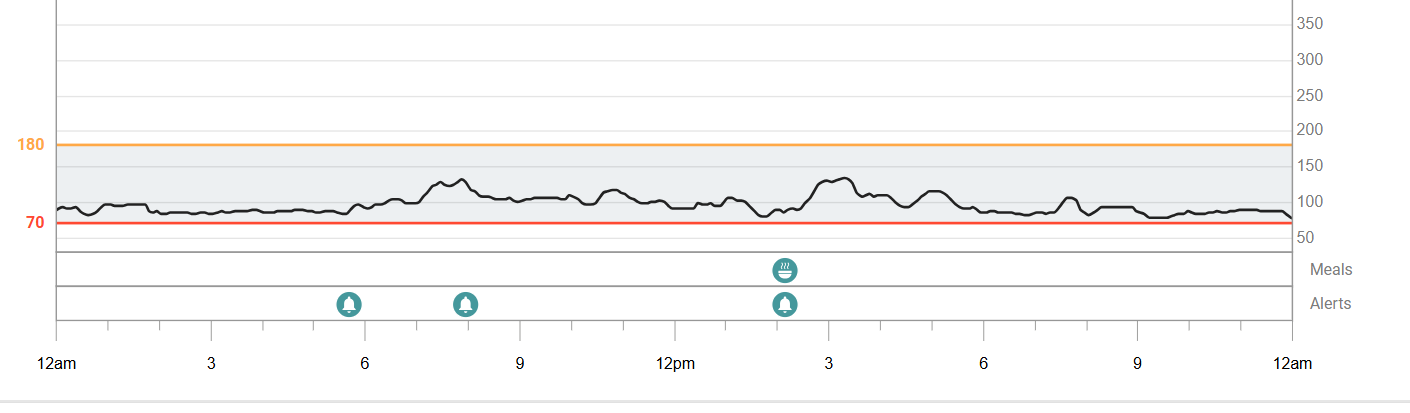
Below are two real glucose traces from real women’s CGMs.
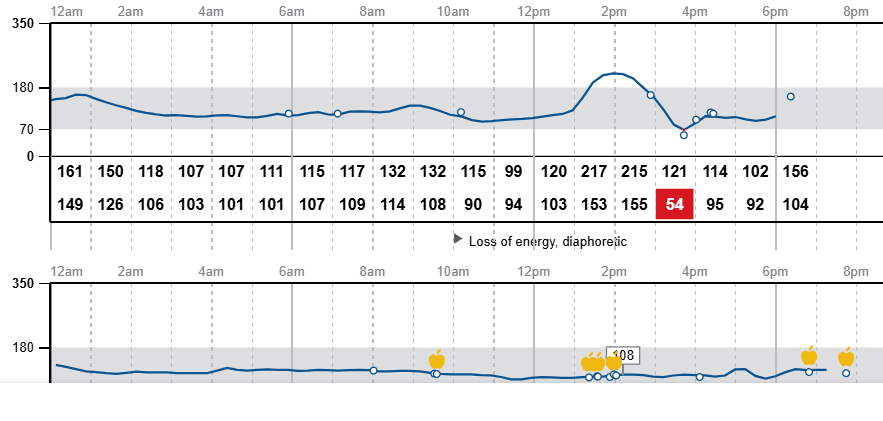
Notice the drop into hypoglycemia after a spike. This spike isn’t too high, but the reactive hypoglycemia is common if the meal had high glycemic foods, insufficient protein, no fiber, and was eaten or absorbed very quickly.
These show something important: blood sugar stability is possible without extreme dieting.
What Stable Blood Sugar Actually Looks Like
When blood sugar is well regulated, glucose gently rises and falls in a smooth wave pattern, typically staying between about 70–120 mg/dL.
In the graphs above you can see:
• gentle rises after meals
• quick recovery back toward baseline
• no extreme spikes or crashes
This is what we want.
Large spikes followed by crashes trigger:
• hunger
• cravings
• cortisol release
• insulin resistance over time.
Note she ate multiple times within the same hour, her blood sugar spiked to 215, then dropped quickly to 54
7 Simple Ways Women Can Buffer Blood Sugar
Many functional medicine strategies focus on buffering the glucose response rather than eliminating carbohydrates completely.
These are strategies for your optimal metabolic health.
1. Start Meals With Protein & Healthy Fat
Eating protein and fat before carbohydrates slows glucose absorption and reduces spikes.
Examples:
• eggs + avocado
• salmon + vegetables
• chicken salad with olive oil
2. Use Apple Cider Vinegar
Acetic acid in vinegar can reduce the blood sugar response to carbohydrate meals. It also aids in digestion. (Avoid or be cautious if you have a history of gastritis or peptic ulcer).
Try:
• 1 tbsp apple cider vinegar in water before meals (drink through a straw to protect your tooth enamel)
• vinegar-based salad dressing
3. Add Cinnamon
Cinnamon may improve insulin sensitivity and slow gastric emptying.
Great on:
• fruit
• yogurt
• oatmeal
4. Eat Fermented Foods
Fermented foods support gut bacteria and help regulate blood sugar signaling.
Examples:
• sauerkraut
• kimchi
• kefir
• yogurt
5. Move Your Body Before or After Eating
Just 10–20 squats or a short walk helps muscles pull glucose out of the bloodstream.
This is one of the fastest ways to reduce a glucose spike.
6. Choose Lower Glycemic Foods
Foods with a lower glycemic index cause slower blood sugar rises. Surprisingly, keto or other no carb diets don’t always lead to healthy and balanced blood sugar. Women often require some form of carbohydrate for blood sugar stability, particularly in our luteal phase or if we are exercising regularly.
Examples:
• berries
• sweet potatoes
• quinoa
• legumes
• pasta made from beans/lentils/chickpeas
• steel cut oats
• cassava
• carrots
• beets
7. Support Micronutrients
Nutrients like chromium play a role in glucose transport into cells and insulin signaling.
This is one reason nutrient density matters for metabolic health.
Why This Matters More for Women
Women often experience cyclical insulin sensitivity. During the luteal phase (the two weeks before your period):
• progesterone rises
• insulin sensitivity drops
• cravings increase
If blood sugar isn’t stable during this phase, symptoms often worsen:
• bloating
• fatigue
• irritability (hello PMS!)
• weight gain
Learning how to buffer glucose can dramatically improve how you feel during these phases.
The Goal Is Stability, Not Perfection
Your blood sugar doesn’t need to be flat. It just needs to be flexible and resilient.
When glucose gently rises and falls like the graphs above, your body can:
• burn fuel efficiently
• regulate hormones
• maintain steady energy
• reduce inflammation